As more members of America’s baby-boom generation become senior citizens, more will come face to face with end-of-life issues:
Should they or their loved ones be allowed to die naturally or kept alive by all means possible?
Should the dying just be made as comfortable as possible or seek treatments with long odds of extending their lives significantly?
Should care or cure, in short, be the overriding concern for seriously ill or dying individuals?
“It’s a transformation process where the person becomes transformed by their illness — becomes a different person, develops a different identity,” Dr. Glen Komatsu, regional chief medical officer for palliative care at Providence Health and Services California, told me last year. “And in some cases, not all, but in many cases patients can come to terms with that new identity and appreciate life for what it’s offering them. It’s a stance of gratitude, awareness, mindfulness. So that’s how we see people who are healed even as they’re dying.”
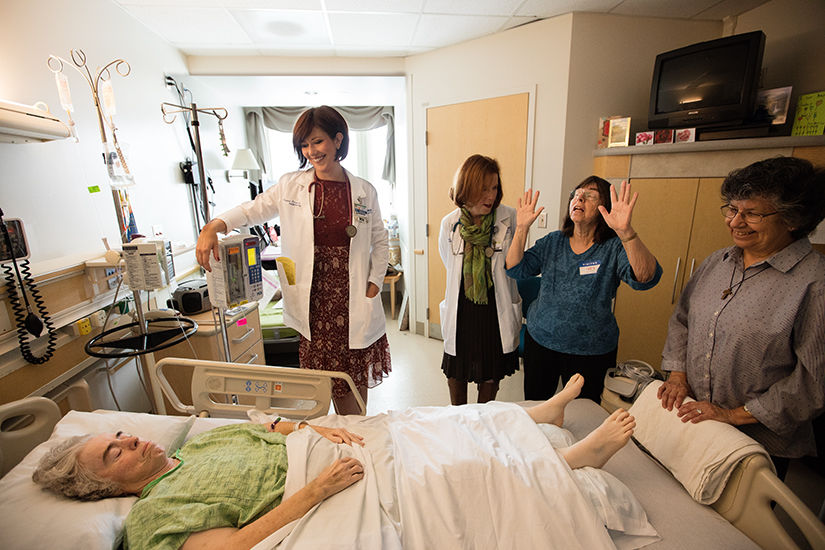
Palliative and hospice programs strive to help patients do just that.
Both have a team approach, made up of physicians, nurses, psychologists, social workers and clergy, to provide not only pain management, but also psychological, social and spiritual support. And these services are tailored to a patient’s particular needs and wishes.
Both work with patients having advanced forms of cancer, serious heart conditions, respiratory diseases, kidney failure, Amyotrophic lateral sclerosis (ALS), multiple sclerosis, Alzheimer’s disease and dementia, and other life-limiting issues as well as those having a poor quality of life because of advanced age.
But there are significant differences, too.
With hospice care, no further efforts are made to cure the patient. Usually, patients have run out of medical options for curing their disease or condition. The other reason is they have decided those options are just too arduous and are likely to cause more harsh symptoms with little likelihood of success.
Moreover, to receive hospice care — and be covered by Medicare, Medi-Cal and private insurance — the patient must be terminal with a diagnosis of six months or less to live.
Palliative care, on the other hand, provides support for patients and their families and “is appropriate at any age and at any stage in a serious illness, and can be provided along with curative treatment,” according to the National Hospice and Palliative Care Organization.
Finally, where hospice programs are often carried out in the patient’s home by visiting hospice workers, palliative care is usually done in a hospital today.
This article originally appeared alongside an article on Dying Well: Pallative Nurses Stress Care Over Curing