Recent headlines about the future of the pro-life movement in the United States — especially with respect to abortion — haven’t been all positive, with some pro-lifers emphasizing the need for better messaging and voter action going forward to protect life in its earliest stages.
But when it comes to end-of-life issues, the movement has a bit more momentum going its way.
For example: Recently, delegates from the extremely influential American Medical Association explicitly rejected physician-assisted killing for the fourth straight time, and also voted down a proposal to rename the practice “medical aid in dying,” a euphemism our Canadian neighbors have deployed with full force.
This maps onto other seemingly improbable victories against physician-assisted suicide and euthanasia in places like England, Ireland, and Denmark, as well as closer to home in New York, Connecticut, and Pennsylvania.
So why are the politics involved in defending life at its end different from doing the same at its beginning?
One clear difference is that progressive disability rights groups have been at the forefront of these end-of-life fights. Their role has made it harder for advocates of euthanasia to argue that their lives are not worth living.
But while pro-lifers are making good progress against attempts to legalize the death of the disabled by action, they’re doing as well against those who are aiming at their death by omission.
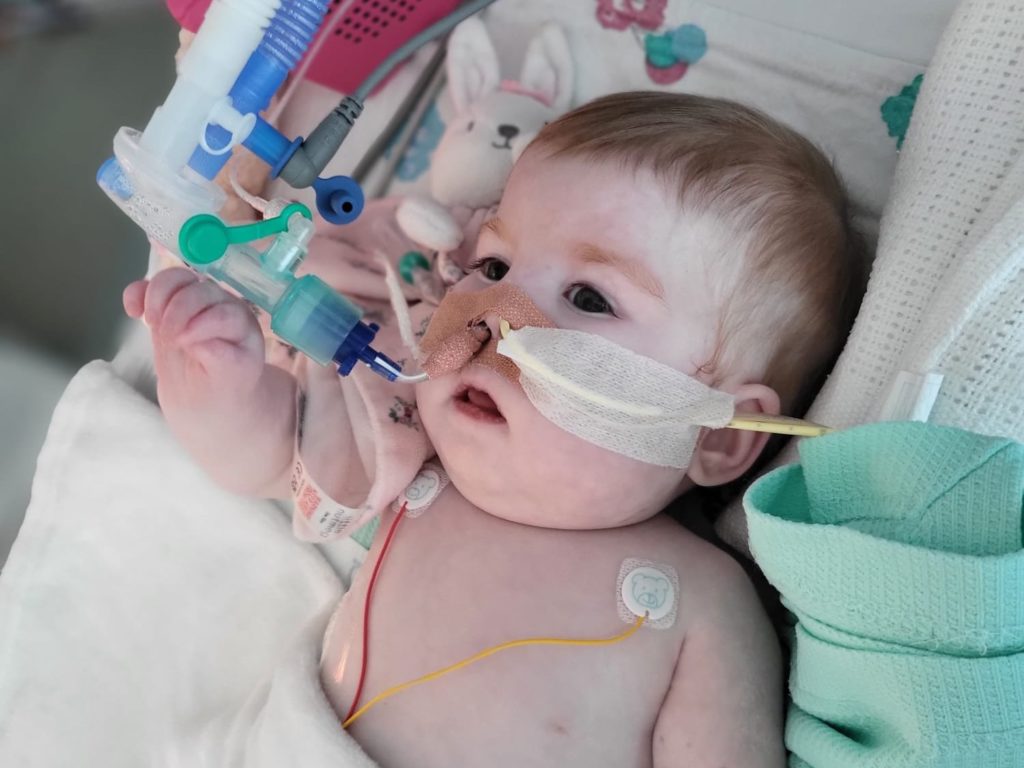
Catholic teaching defines euthanasia as an act or omission which of itself or by intention causes death, a definition that calls to mind the tragic story of Baby Indi in the United Kingdom, the most recent child in a growing list to be euthanized against the will of her parents.
In such cases, both the medical teams and the judges have insisted that the child is so disabled that their lives are no longer worth living. They are so confident in this judgement that they deem the parents’ desire for their child to continue to live as constituting a kind of child abuse.
To add insult to injury, the judges ruled that Baby Indi’s life support had to be administered at a hospital or hospice and not at the child’s home as the family desired — pretty much implying that the parents want to abuse their own child.
Of course, someone — even a Catholic — might ask: What’s the big deal with removing the child’s life support? Does not even the Catholic Church allow for the removal of extraordinary means of medical treatment in such cases?
The answer is: it depends.
If one is not aiming at death, but rather at removing burdensome, life-sustaining treatment, the Church leaves this option wide open.
After all, it’s also possible to make an idol out of grasping for more life. In our religious tradition, the images and narratives of Jesus’ death — and the deaths of martyrs — represent central examples of Christian sanctity. Choosing to live one’s final days or hours without life-sustaining treatment, far from being wrong, can be a holy and beautiful choice.
This, however, was nothing close to what the decision-makers in Baby Indi’s case had in mind. The key lies in analyzing what is being aimed at here: What was the intention of the medical team and the judges?
If they had simply claimed that the intensive care itself was so overwhelmingly burdensome that it represented a kind of child abuse, then they would have an argument. But the actual reasoning used in the case reveals that this is not what was going on.
Consider their assessments of Baby Indi’s disabilities: “There is no discernible quality of life or interaction by IG with the world around her.” “She has extremely limited quality of life.” “She seems to derive comfort from M stroking her hair, but I accept the clinical observations that she does not follow with her eyes, does not respond to stimuli, and her limb movements are not purposeful. I do not think she experiences any meaningful quality of life, and sadly she never will.”
Those judges determined that Indi had just enough awareness to experience the difficulties of intensive care, but not enough to have “meaningful” quality of life.
Interestingly, these are precisely the kinds of judgments that disability rights activists are so worried about.
Suppose, for example, that Baby Indi had life support removed but continued to breathe and live. Would the medical team and judges be pleased with this outcome?
Based on their assessment, they wouldn’t be. Instead, they made a judgment that Indi’s life was not worth living, revealing what was really at play here: an omission intended to cause death, an example of the passive euthanization of a disabled child.
Sadly, once one starts paying attention to similarly aimed omissions — including in U.S. health care settings — we reach the unfortunate conclusion that this kind of child euthanasia happens quite regularly.
Yes, there are good reasons for hope in the struggle against aiming for the death of the disabled by action. But the very same reasoning and concern for justice for the disabled should be applied when aiming at death that happens by omission, too.
The very public cases of those like Baby Indi’s serve as a wake-up call: let those with eyes, see, and those with ears, hear — and then act accordingly.