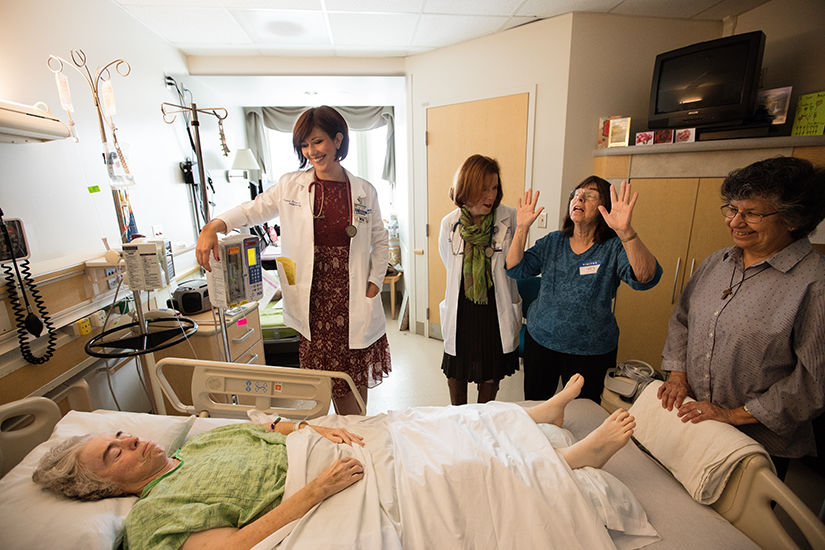
After putting on yellow hospital gowns over their white jackets, three nurses from the palliative care team at Providence Little Company of Mary Medical Center in Torrance walked into room 497.
“How are you doing?” asked Marianne Ayala, nurse manager of the team, kneeling on the side of Roselia Nu√±ez’ bed. Looking up, the elderly patient forced a small smile.
Nurse practitioner Salve Bautista checked her vital signs, while nurse Rebekah Riemer comforted her.
After a few minutes, Ayala went over to Nu√±ez’ daughter, Isabel Uribe, who was standing nearby in the small rectangular room. They talked quietly about a wound infection her mother had developed from recent surgery.
The daughter said she would like the doctor involved to call her brother in San Bernardino to explain the dwindling medical options left for their mother, who had congestive heart failure as well as being diabetic and anemic.
Certain treatment options could extend her life, but could also further her suffering.
“I don’t want to make that decision to shut things down,” said the daughter, tears welling in her eyes.
Ayala nodded.
“I’m not God. I’m not God. I know I’m going to die. If I have cancer, I’m willing to die. But God has made that choice, not me.”
“It’s not you,” Ayala repeated. “It’s not you.”
“And on the other hand, I don’t want to see her suffer, either.”
Ayala put an arm around Uribe’s shoulder. “I know. I know.”
Crying now, the young woman said, “It’s very hard to do this. It’s not easy. It’s not easy. It’s not like other decisions in life. Buying something. Ordering a drink. Buying a home. It’s not the same.”
“No, it’s not the same,” Ayala almost whispered. “It’s not the same.”
A ‘gentler’ approach
Earlier, the managing palliative care nurse had told me the most challenging cases are patients who are clearly at the end of life and would really benefit from a “gentler” approach like hospice.
During hospice care, which is often done in the patient’s home through a visiting hospice nurse and family caregiver, all treatments such as chemotherapy, surgery and lab works are usually stopped. So with most programs, the patient is expected to live only six months or less. Making the dying person as comfortable as possible becomes the focus.
Many times today, says Ayala, there are situations where gravely ill patients can’t speak. And they have not filled out an advanced directive. The directive specifies their end-of-life medical wishes, or gives power of attorney or health care proxy to make decisions when they are incapacitated. So these seriously sick individuals often wind up in a hospital’s ICU (intensive care unit) connected to all kinds of tubes and machines.
“We see what the path ahead is going to be,” she said. “We know that the treatments that are being given or offered are futile. The patient is not predicted to survive or have any better quality of life.
“And yet families — just the way medicine is practiced now — have to decide oftentimes whether to continue these aggressive treatments. So I think we put families in a really hard place because of that. There’s something to be said for doctors making recommendations and families taking them into consideration. But often we see families who become extremely resistant to that. It’s like they know better, and they’re going to keep treatments going for however long they can.”
After a moment, she added, “So that is hard to see. What we see looks like suffering, which is hard to tell at times, but it looks to be the patient is suffering. But the family, because of their own suffering, will not deal with a lot of our counseling and are really resistant. So for me, that’s the hardest thing.”
‘At peace’
The three nurses were all smiling again coming into Linda Fisher’s room. The 75-year-old with gray curly hair smiled back. This time it was Rebekah Riemer who bent down beside her bed, putting a hand on the woman’s shoulder.
Ayala asked if she was in much pain. Fisher, shaking her head, smiled again.
Riemer leaned a little closer. “When I met you for the first time, I think within the first five minutes you expressed to me how important your faith and your relationship with Jesus was,” she said.
The patient nodded.
“When I asked you how you were doing, you said you were at peace. Absolutely.”
Another nod.
“That was just incredible to give your family there and to us — knowing that you were at peace. And I think that your message has been heard by so many people who work here at Little Company of Mary. So we thank you for that.”
After a moment, Riemer asked, “Have you any concerns about how everything is going with your care?”
“You’ve done so much with the pain,”
Ayala said, “I’m really glad that we could do that.”
“Yes, you’ve done enough.”
Suddenly the patient rose up in her bed, eyes closed, pointing to the ceiling. “He will raise us up again. You need to love, worship daily. You should pray to God daily. And Jesus just lifts me up in the valley of the shadow of death. And I think Jesus is everywhere,” she said. “So I’m ready to see him.”
“You inspire us,” said Ayala.
“Absolutely,” agreed Riemer
“And give us hope,” added Ayala.
Dying well
In the palliative care center’s conference room before our patient visits, I’d asked the three palliative nurses on the team if people could really “die well”? It just seemed like such a contradiction.
“Oh, yes,” came back Ayala. “I would say absolutely, yes. I think that dying well for patients and for their loved ones means dying in a way that is aligned with their goals and preferences. And so that’s really a hallmark of what we try to accomplish in palliative care is helping families discern what those goals and preferences and values are. And then it’s trying to set up a support system or situation where that can happen.”
She says for some patients and their families a good death might mean doing everything possible to keep them alive. And the palliative team respects that as well.
“But typically a good death is, I think, where patients have at least acknowledgement and understanding of what’s happening,” she explained. “People are able to have their families and loved ones around them. People are able to say the things that they need to say to each other. So we try to foster that.”
Ayala also believes a good death can actually be a time of real personal growth.
“I think it’s a state of transformation,” she said. “It’s like the birthing process. It’s a process. And people go through it very differently. But I think it can be an opportunity for those who are self-aware or open to it. I don’t think that happens for everyone by any means.
“But we’ve witnessed growth,” she reported. “And that’s really beautiful when it happens. I don’t know how else to describe it.”
The other nurses were nodding.
“Death itself in our society is just considered not good because it takes away from what is known and kind of brings you to the unknown,” said Bautista. “But I would define a good death as when a patient would say, ‘I have lived a full life,’ and they’re not dreading whatever may be.
“And sometimes patients need to do some processing, you know, trying to reach out to prepare for what that next stage would be. And so this stage of pain, transition, I believe truly is a time of growth. I would define it as a good death.”
Some of the most fulfilling and peaceful deaths Bautista has seen have been with patients who not only accept their own dying process but also accept the way they’ve lived their lives. And along with that, she has witnessed profound personal growth.
“It’s amazing to see families that were once estranged come together and make decisions that are right for their loved ones,” she said. “But that doesn’t happen every time. We wish it would. But just seeing people break through barriers they might not have been able to break through — especially with loved ones and relationships — just coming to grips and peace at the end of life is wonderful.”
Emotional suffering, too
On that recent Wednesday morning, we walked across the street to the transition care center with a hospice unit. The patient we were visiting came from another hospital in terrible chronic pain. Providence Little Company of Mary’s palliative team helped Ernesto Kabigting transition to hospice care and greatly lessen his pain.
“Hi! Hi, Eddie!” said Bautista, going to his bedside.
Ayala asked, “How are you?”
The elderly Filipino man said, “I’m fine,” sitting up a little. But concern was all over his weathered face. And he looked like he had been crying.
“Oh, it’s so good to see you,” she said.
The patient nodded, and the group was off making small talk.
After a few minutes, the subject of pain came up. And Kabigting started speaking in an agonizing voice. “I was looking for my pain when I came here,” he said, running a hand around his neck, down his chest all the way to his legs. “And it’s hard to explain. All down my body. I was screaming every night, ‘What am I going to do?’ I didn’t want to wake up because of the pain. Pain all over."
“But since I’ve been here, now pain all gone,” he said. “I can spend time with some of my family. So it’s good. It’s better now.” Yet, his eyes still glistened.
Walking back to the hospital, Bautista said that when he came to Little Company of Mary he hadn’t slept in weeks because of being in constant agony. Doctors only recently diagnosed that his lung cancer had spread throughout the bones of his frail body, causing him unbearable suffering.
“Now that his physical pain is better controlled, he’s talking about a different pain,” she noted. “And we see this with a lot of our patients in palliative care, where the physical pain is but a part of the total pain that they’re feeling. The pain is the short time he has left, but he says he’s at peace with that. But there’s a pain associated with not being with his whole family. Some are in Canada, others in the Philippines.
“The only family members who are supporting him here are one daughter and a cousin. But he does not want to be a burden to them, either. So he was talking to me more about the emotional pain that he’s going through right now.”
I asked about a dream he had told her before we left. Bautista half-smiled. “He was in a field with a lot of sheep,” she said. “And instead of him trying to find the sheep to shepherd, what he found was himself. As if he was the sheep that needed shepherding.”
More info on end-of-life care in this related article: Pallative vs.Hospice Care